Missing teeth affect far more than your smile’s appearance — they influence chewing ability, speech clarity, and the long-term health of the jaw. Dental implants restore a tooth from root to crown, providing a foundation that mirrors natural tooth function. Unlike removable options, implants integrate with the jawbone to offer stability that supports everyday activities with confidence and comfort.
Advances in materials and imaging mean implants are predictable, durable solutions for a wide range of needs. With careful planning and modern surgical techniques, implants can replace a single tooth, stabilize a denture, or support an entire arch. For many patients, the result is a restoration that looks, feels, and performs much like their original teeth.
Choosing the right treatment starts with an evaluation that considers your oral health, bone volume, and long-term goals. A tailored approach ensures the implant solution aligns with your lifestyle — whether you want a discreet single crown or a full-arch restoration designed for permanence and function.

At their core, implants are biocompatible posts placed into the jaw to replace the tooth root. Once the implant integrates with bone, it acts as a secure anchor for a prosthetic tooth — a crown, bridge, or denture — restoring chewing mechanics and preserving facial structure. This root-level support is what distinguishes implants from prosthetics that rely on surrounding teeth or soft tissue.
Because implants transfer biting forces into the jaw, they help maintain bone volume and the natural contour of the face. That structural preservation reduces the long-term changes that can occur after tooth loss, contributing to both functional and aesthetic benefits that extend beyond the immediate restoration.
Successful implant care begins with detailed planning. Diagnostic imaging, including three-dimensional scans when appropriate, helps the clinical team evaluate bone quality, anatomical landmarks, and precise implant placement. A comprehensive plan may also consider whether preliminary treatments — such as extractions or bone grafting — are needed to create a reliable foundation.
During consultations, your clinician will discuss appropriate anesthesia and any comfort measures to make the procedure manageable. Treatment sequencing and the timeline for temporary or final restorations are shared up front so you know what to expect during each phase of care. Thorough communication throughout helps reduce uncertainty and supports better outcomes.
Implant placement is typically completed as an outpatient procedure. After the post is set in the jaw, a period of healing follows while bone grows around the implant — a process called osseointegration. Depending on the case, temporary teeth can sometimes be placed the same day, while other situations call for a healing interval before attaching the final restoration.
Once integration is secure, restorative components are fabricated to match surrounding teeth in shape and color. The final result is designed to be functional and natural in appearance. Post-operative instructions and follow-up appointments help ensure healing proceeds smoothly and that your new restoration integrates comfortably into daily life.
Implant dentistry is flexible. A single implant topped with a crown replaces one missing tooth without altering adjacent teeth. For several missing teeth, implant-supported bridges offer a way to reconstruct gaps while preserving neighboring structures. Full-arch restorations, supported by a series of strategically placed implants, can replace an entire dental arch with strength and stability that closely replicates natural dentition.
For denture wearers, implant-retained dentures provide a marked improvement in function and comfort. These overdentures attach to implants to prevent slipping and to give better chewing efficiency. The range of options allows clinicians to design a plan that balances patient preferences, anatomical conditions, and long-term goals.
The number and placement of implants depend on factors like bone availability, bite forces, and aesthetic demands. Clinicians weigh these elements to determine whether a single implant, an implant-supported bridge, a fixed full-arch prosthesis, or an implant-retained denture is the best choice. Each configuration has predictable benefits when paired with meticulous planning and execution.
When appropriate, immediate provisional teeth can be provided to restore appearance and function while the implants integrate. The final restoration is then crafted to deliver an optimal balance of durability, comfort, and natural-looking form.
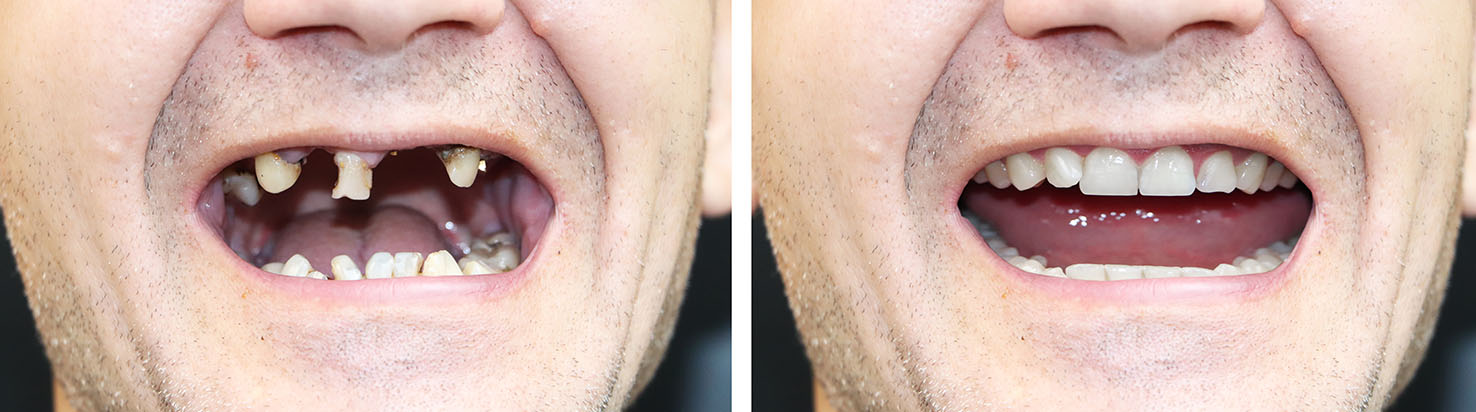
Long-term implant success depends on adequate bone to stabilize the implant. When teeth are lost, the supporting bone can resorb over time. If bone volume is insufficient, grafting techniques can rebuild the site to accept implants. Bone grafts can use sterile graft materials or, in some cases, a patient’s own bone to create a robust environment for integration.
Soft tissue health is also important. Healthy gums support aesthetic outcomes and help protect the implant-restoration interface. Clinicians may recommend periodontal care or soft-tissue augmentation to optimize both the appearance and longevity of the final restoration.
Modern implant protocols, combined with precise imaging and careful surgical technique, have led to high success rates. When performed and maintained appropriately, implants provide reliable, long-term function. Regular follow-up visits and consistent oral hygiene are integral parts of preserving implant health over the years.
Patients with certain medical conditions or habits may require additional evaluation prior to treatment. During your assessment, the clinical team will review your medical and dental history to identify any factors that could affect planning or healing and will tailor recommendations accordingly.
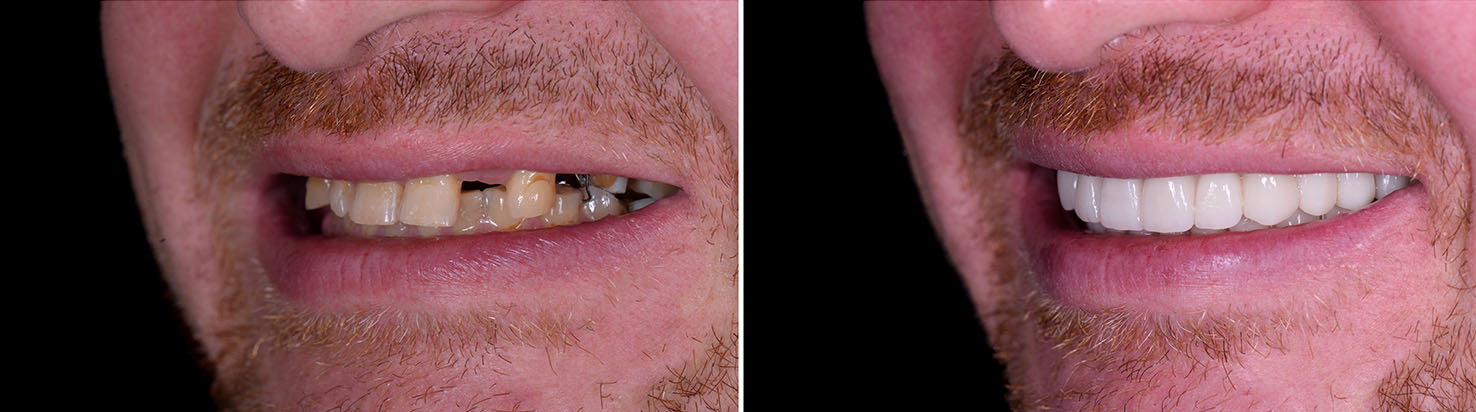
Once your implant restoration is in place, daily oral hygiene practices — brushing, flossing, and using interdental tools where appropriate — help prevent problems around the implant. Just as with natural teeth, plaque control and routine cleaning are essential. Many patients find that a combination of electric brushing and targeted interdental cleaning makes maintenance straightforward.
Professional maintenance visits allow clinicians to monitor tissue health, check the integrity of implant components, and perform any necessary cleanings that are difficult to accomplish at home. Early detection of changes makes it possible to address issues before they progress.
After surgery, follow-up appointments are scheduled to evaluate healing and to guide the transition to final restorations. Over the long term, periodic checkups help confirm that tissues remain healthy and that restorations function as intended. If you notice changes in how your restoration feels, experience discomfort, or detect any unusual swelling, contacting your dental team promptly allows them to assess and advise on next steps.
Dental implants offer predictable, long-lasting solutions for replacing missing teeth and restoring oral function. If you would like to explore whether implants are the right choice for your situation, the team at Diamond Head Dental Care can evaluate your needs and outline a personalized plan. We focus on careful planning, clear communication, and results that support both health and confidence.
To learn more or to schedule an evaluation, please contact us for additional information. We’re happy to answer questions and guide you through the next steps toward rebuilding a comfortable, natural-feeling smile.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are biocompatible posts placed in the jaw to replace missing tooth roots and provide stable support for a prosthetic tooth. Once the implant integrates with the surrounding bone through osseointegration, it acts as an anchor for a crown, bridge, or denture to restore chewing and speech. This root-level support helps preserve jawbone volume and facial contours in ways that removable prosthetics cannot.
Implants are designed to mimic the mechanics and appearance of natural teeth, transferring bite forces into the jaw to maintain bone health. Modern materials and imaging techniques make placement predictable and precise, improving both function and aesthetics. When planned and executed carefully, implants deliver long-term, natural-feeling results that integrate seamlessly with remaining teeth.
Good candidates typically have adequate jawbone volume, healthy gum tissues, and a commitment to oral hygiene and regular dental visits. The clinical team will review your medical and dental history to identify conditions or habits, such as uncontrolled systemic disease or tobacco use, that may require additional evaluation or preparatory treatment. A thorough examination and diagnostic imaging help determine whether implants are the best option for your needs.
Many patients who were previously told they were not candidates can now pursue implants with modern grafting and augmentation techniques. If preliminary treatments like extractions, periodontal therapy, or bone grafting are needed, they are incorporated into a tailored plan to create a stable foundation. Shared decision-making ensures the chosen approach aligns with your health, function, and aesthetic goals.
Preparation begins with a comprehensive consultation, diagnostic imaging, and a review of your medical history to plan safe and precise implant placement. Your clinician will discuss recommended preoperative steps, which may include completing dental infections or periodontal care, arranging for any needed grafting, and following instructions about medications and fasting when sedation is planned. Clear communication about anesthesia options and comfort measures helps you arrive prepared and confident for the procedure.
Maintaining good oral hygiene in the weeks before surgery supports optimal healing and reduces infection risk. If you have health conditions such as diabetes or take medications that affect healing, your provider will coordinate with your physician as needed to minimize risks. Practical preparations, like arranging transportation after sedation and planning for a short recovery period, make the day of surgery smoother.
The implant process typically follows staged steps that include evaluation, surgical placement, a healing period for osseointegration, and final prosthetic restoration. Some cases allow for temporary teeth or immediate provisional restorations, while others require a healing interval before attaching the definitive crown or bridge. Throughout treatment, the team will explain anticipated timelines, milestones, and follow-up visits so you know what to expect at each phase.
Diagnostic imaging and careful planning determine the exact sequence and timing, and any necessary adjunctive procedures are scheduled before or during placement to achieve a durable result. Regular follow-up during the healing period allows clinicians to monitor integration and tissue health and to address any concerns promptly. The office of Diamond Head Dental Care emphasizes clear communication and individualized scheduling to balance function, comfort, and esthetics.
Implant dentistry offers a range of solutions from single-tooth implants to implant-supported bridges and full-arch restorations, enabling clinicians to match treatment to each patient s needs. Single implants restore an individual tooth without altering adjacent teeth, while implant-supported bridges can replace several teeth with fewer implants than individual replacements. For patients missing a full arch, fixed prostheses or implant-retained overdentures provide stability and improved chewing compared with conventional dentures.
The choice of configuration depends on factors such as bone quality, bite dynamics, aesthetic goals, and patient preferences. Immediate provisional restorations may be possible in appropriate cases to restore appearance and function during healing. Your clinician will review the benefits and trade-offs of each option and recommend the plan most likely to provide lasting, comfortable results.
Bone grafting is recommended when there is insufficient jawbone volume to support an implant safely and predictably, which can occur after long-standing tooth loss or periodontal disease. Grafting rebuilds the site using sterile graft materials or, in select cases, the patient s own bone to create a stable foundation for implant placement. Soft tissue augmentation may also be advised to improve gum thickness and the aesthetic outcome around the restoration.
Advanced imaging helps determine the extent of deficiency and the most appropriate grafting technique, which may be staged before implant placement or performed at the time of surgery. When performed with proper planning and technique, these procedures increase the likelihood of successful integration and long-term stability. Your clinician will explain the rationale, expected healing, and how grafting fits into the overall treatment timeline.
Dental implants are designed for long-term function and can last many years or decades when placed correctly and maintained with good oral hygiene. Success depends on factors such as the quality of the bone, the accuracy of implant placement, the patient s oral hygiene habits, and regular professional maintenance. Lifestyle factors and systemic health conditions that affect healing may influence long-term outcomes and are evaluated during planning.
Routine follow-up visits allow clinicians to monitor the implant components and surrounding tissues, make adjustments if needed, and address early signs of problems. Wear of the prosthetic components can occur over time and surface maintenance or replacement may be needed to preserve function and appearance. A consistent home-care routine and periodic professional care help protect your investment in implant-supported teeth.
Daily plaque control is essential for implant health and includes thorough brushing, interdental cleaning with floss or interdental brushes, and attention to the contact points around the restoration. Many patients find an electric toothbrush combined with targeted interdental tools simplifies routine care and helps maintain healthy gum tissues. Avoiding habits that place excessive forces on implants, such as chewing very hard objects, also supports long-term success.
Professional maintenance visits allow clinicians to assess tissue health, clean areas that are difficult to reach at home, and check the integrity of the implant components. Early detection of tissue changes, loosening, or wear enables timely intervention before problems progress. Your dental team will recommend a personalized recall schedule based on your risk profile and the type of restoration in place.
As with any surgical procedure, implant placement carries risks that include infection, impaired healing, and, in rare cases, nerve or sinus involvement depending on the implant site. Meticulous planning, imaging, and surgical technique reduce these risks, and preoperative evaluation helps identify medical or local factors that may necessitate modified care. If issues arise after surgery, prompt assessment and treatment increase the chances of a favorable resolution.
Possible complications such as peri-implant inflammation or component loosening are typically managed with targeted hygiene measures, professional cleaning, or restorative adjustments. In uncommon cases of implant failure, removal and site rehabilitation are options to restore function with an alternative approach. Open communication with your clinician and adherence to follow-up recommendations help minimize complications and support long-term implant health.
Getting started begins with a comprehensive consultation that includes a dental and medical history review, clinical examination, and diagnostic imaging to evaluate bone volume and anatomical considerations. During this visit the clinician will discuss treatment goals, outline possible implant options, and explain the anticipated sequence of care, comfort measures, and follow-up schedule. This planning visit ensures recommendations are personalized and aligned with your functional and aesthetic priorities.
The consultation also covers whether preliminary treatments like periodontal therapy, extractions, or grafting are needed to achieve predictable results and how those steps fit into the overall timeline. The team at Diamond Head Dental Care welcomes questions and will explain each phase of care so you can make an informed decision about restoring your smile. When you are ready, the practice will coordinate the diagnostic work and schedule the treatment plan that best meets your needs.
